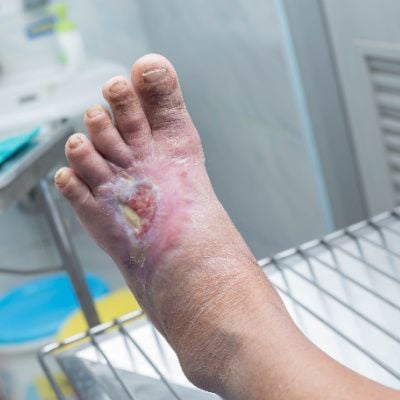
 Foot ulcers, though seemingly innocuous at first glance, can pose serious health risks and complications, especially for individuals with underlying conditions. In this comprehensive guide, we delve into the intricacies of foot ulcers, exploring their causes, symptoms, and the imperative need for effective management strategies.
Foot ulcers, though seemingly innocuous at first glance, can pose serious health risks and complications, especially for individuals with underlying conditions. In this comprehensive guide, we delve into the intricacies of foot ulcers, exploring their causes, symptoms, and the imperative need for effective management strategies.
Understanding Foot Ulcers
Foot ulcers are open sores or wounds that typically develop on the feet, particularly on the bottom. These ulcers can penetrate deep into the skin layers, exposing underlying tissues. While anyone can develop a foot ulcer, they are more prevalent among individuals with conditions such as diabetes, peripheral neuropathy, or vascular diseases.
Causes of Foot Ulcers
-
Diabetes: Individuals with diabetes often experience neuropathy (nerve damage) and reduced blood circulation, making them more susceptible to foot ulcers. Elevated blood sugar levels contribute to delayed wound healing.
-
Peripheral Artery Disease (PAD): Reduced blood flow to the extremities, a common feature of PAD, can lead to poor wound healing, increasing the risk of ulcers.
-
Peripheral Neuropathy: Nerve damage in the feet, often associated with conditions like diabetes, diminishes the sensation, making it challenging to detect injuries or friction that can evolve into ulcers.
-
Foot Deformities: Structural abnormalities or deformities, such as bunions or hammertoes, can create increased pressure, predisposing the foot to ulcers.
-
Trauma or Injury: Direct injury, burns, or repeated friction, especially in ill-fitting footwear, can break the skin barrier and initiate ulcer formation.
Recognizing Symptoms: Early Indicators of Foot Ulcers
-
Pain or Discomfort: Individuals may experience persistent pain or discomfort, often disproportionate to the size of the ulcer.
-
Drainage or Pus: Open sores may produce drainage or pus, indicating infection.
-
Redness and Swelling: The surrounding skin may exhibit redness and swelling, reflecting inflammatory processes.
-
Odor: Infected ulcers can emit an unpleasant odor, signaling the presence of bacteria.
-
Delayed Healing: Ulcers that do not show signs of improvement or continue to worsen require prompt attention.
Effective Management Strategies
-
Wound Care: Thorough cleaning and dressing of the ulcer are paramount. Dressings that maintain a moist environment facilitate healing.
-
Offloading Pressure: Minimizing pressure on the ulcer through customized footwear, braces, or crutches helps prevent further damage.
-
Infection Control: Antibiotics may be prescribed to address or prevent infection. Timely intervention is crucial to avoid complications.
-
Blood Sugar Control: For individuals with diabetes, maintaining optimal blood sugar levels is essential for fostering efficient wound healing.
-
Vascular Interventions: Individuals with compromised blood flow may benefit from vascular procedures or interventions to improve circulation.
-
Regular Monitoring: Consistent monitoring of the ulcer's progress, coupled with routine foot inspections, helps identify issues early on.
The Role of Prevention
Prevention plays a pivotal role in mitigating the risk of recurrent foot ulcers:
-
Proper Foot Hygiene: Regular washing and inspection of the feet can prevent minor issues from escalating into ulcers.
-
Footwear Choices: Opting for well-fitted, supportive shoes can reduce friction and pressure, minimizing the risk of ulcer development.
-
Routine Check-ups: Regular visits to healthcare professionals for foot assessments are crucial, especially for individuals with diabetes or vascular conditions.
Conclusion
In conclusion, understanding the complexities of foot ulcers empowers individuals to take proactive steps in their foot health journey. Whether spurred by diabetes, neuropathy, or other contributing factors, early detection and effective management are pivotal for successful outcomes. By adopting preventative measures, seeking timely medical attention, and fostering a holistic approach to foot care, individuals can navigate the challenges of foot ulcers and pave the way for enhanced well-being and mobility.
Disclaimer:
The information on this website is provided for educational and information purposes only and is not medical advice. Always consult with a licensed medical provider and follow their recommendations regardless of what you read on this website. If you think you are having a medical emergency, dial 911 or go to the nearest emergency room. Links to other third-party websites are provided for your convenience only. If you decide to access any of the third-party websites, you do so entirely at your own risk and subject to the terms of use for those websites. Neither Foot Care Center, nor any contributor to this website, makes any representation, express or implied, regarding the information provided on this website or any information you may access on a third-party website using a link. Use of this website does not establish a doctor-patient relationship. If you would like to request an appointment with a health care provider, please call our office at 4027217171.


