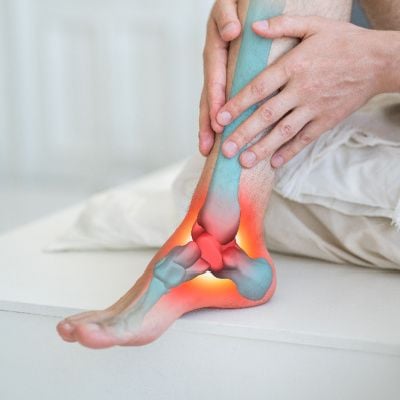
 Osteoarthritis, the most prevalent form of arthritis, can affect various joints throughout the body, including the intricate structures of the foot and ankle. This degenerative joint condition, often associated with wear and tear, can significantly impact an individual's mobility and quality of life. In this comprehensive guide, we will delve into the complexities of osteoarthritis of the foot and ankle, exploring its causes, symptoms, diagnostic methods, and effective management strategies. Understanding this condition is paramount for individuals seeking insights into their foot health and for healthcare professionals aiming to provide targeted care.
Osteoarthritis, the most prevalent form of arthritis, can affect various joints throughout the body, including the intricate structures of the foot and ankle. This degenerative joint condition, often associated with wear and tear, can significantly impact an individual's mobility and quality of life. In this comprehensive guide, we will delve into the complexities of osteoarthritis of the foot and ankle, exploring its causes, symptoms, diagnostic methods, and effective management strategies. Understanding this condition is paramount for individuals seeking insights into their foot health and for healthcare professionals aiming to provide targeted care.
Understanding Osteoarthritis
What is Osteoarthritis?
Osteoarthritis is a degenerative joint disorder characterized by the gradual breakdown of cartilage, the protective tissue covering the ends of bones. As this cartilage wears away, bones may rub against each other, causing pain, stiffness, and reduced joint mobility.
The Foot and Ankle's Role
The foot and ankle, with their intricate network of joints, ligaments, and tendons, are susceptible to osteoarthritis due to the constant pressure and strain they endure in daily activities such as walking and standing.
Causes of Osteoarthritis in the Foot and Ankle
Age and Wear
Advancing age is a primary risk factor for osteoarthritis, as the cumulative effects of wear and tear on joints become more pronounced over time.
Genetics and Hereditary Factors
Genetic predisposition can contribute to an individual's susceptibility to osteoarthritis. Family history of the condition may increase the likelihood of its development.
Joint Instability and Injury
Previous injuries or conditions that affect the stability of the foot and ankle joints, such as ligament tears or fractures, can elevate the risk of osteoarthritis.
Recognizing Symptoms of Foot and Ankle Osteoarthritis
Joint Pain and Stiffness
Persistent pain, particularly after periods of inactivity, and stiffness in the affected joints are hallmark symptoms of osteoarthritis.
Swelling and Tenderness
Inflamed joints may exhibit swelling and tenderness, further limiting mobility and causing discomfort.
Reduced Range of Motion
Individuals with foot and ankle osteoarthritis may experience a gradual decrease in their range of motion, impacting activities such as walking and climbing stairs.
Diagnosing Foot and Ankle Osteoarthritis
Clinical Evaluation
Healthcare professionals conduct a thorough examination, assessing the affected foot and ankle for signs of tenderness, swelling, and joint function.
Imaging Studies
X-rays, MRIs, or CT scans may be ordered to visualize the extent of joint damage, cartilage loss, and the presence of bone spurs, characteristic of osteoarthritis.
Joint Aspiration
In cases where the diagnosis is unclear, joint aspiration, involving the removal and analysis of synovial fluid, can help confirm the presence of osteoarthritis.
Stages of Foot and Ankle Osteoarthritis
Early Stage
Mild joint pain, occasional stiffness, and minimal impact on daily activities characterize the early stage of osteoarthritis.
Moderate Stage
As osteoarthritis progresses, joint pain becomes more persistent, swelling may occur, and daily activities may be noticeably affected.
Advanced Stage
Severe pain, significant joint deformity, and a substantial reduction in mobility mark the advanced stage of foot and ankle osteoarthritis.
Management Strategies for Foot and Ankle Osteoarthritis
Lifestyle Modifications
Weight management, adopting joint-friendly exercises, and choosing appropriate footwear are fundamental for minimizing stress on affected joints.
Physical Therapy
Tailored exercises designed to improve joint flexibility, strengthen supporting muscles, and enhance overall foot function are central to managing osteoarthritis.
Medications
- Pain Relievers: Over-the-counter or prescription medications, such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs), help manage pain.
- Topical Treatments: Creams or patches containing NSAIDs or capsaicin can provide localized relief.
Assistive Devices
Orthotic inserts, braces, or custom footwear can offer additional support, redistribute weight, and alleviate pressure on affected joints.
Injections
Corticosteroid injections may be recommended for their anti-inflammatory properties, providing temporary relief from pain and swelling.
Surgical Intervention
In severe cases, surgical options such as joint fusion or joint replacement may be considered to address advanced joint degeneration.
Living with Foot and Ankle Osteoarthritis
Coping Strategies
Developing coping mechanisms, including stress reduction techniques and seeking emotional support, is essential for managing the impact of osteoarthritis on daily life.
Patient Education
Empowering individuals with knowledge about their condition, treatment options, and self-care practices enables them to actively participate in their care.
Seeking Professional Guidance
Podiatrists and Orthopedic Specialists
Consulting with healthcare professionals specializing in foot and ankle conditions ensures accurate diagnosis, personalized treatment plans, and ongoing monitoring.
Pain Management Specialists
In cases of severe pain, collaboration with pain management specialists can provide targeted interventions and additional pain relief strategies.
Conclusion
In conclusion, understanding osteoarthritis of the foot and ankle is crucial for individuals navigating this common yet challenging condition. By adopting a multifaceted approach that includes lifestyle modifications, targeted therapies, and professional guidance, individuals can effectively manage symptoms, preserve joint function, and enhance their overall quality of life. Embracing a proactive stance toward foot and ankle health empowers individuals to thrive despite the challenges posed by osteoarthritis, fostering a sense of well-being and mobility.
Disclaimer:
The information on this website is provided for educational and information purposes only and is not medical advice. Always consult with a licensed medical provider and follow their recommendations regardless of what you read on this website. If you think you are having a medical emergency, dial 911 or go to the nearest emergency room. Links to other third-party websites are provided for your convenience only. If you decide to access any of the third-party websites, you do so entirely at your own risk and subject to the terms of use for those websites. Neither Foot Care Center, nor any contributor to this website, makes any representation, express or implied, regarding the information provided on this website or any information you may access on a third-party website using a link. Use of this website does not establish a doctor-patient relationship. If you would like to request an appointment with a health care provider, please call our office at 4027217171.


